Scientists Shed Light on How Stressed Cells Sequester Protein-Forming mRNAs
Researchers at Weill Cornell Medicine have illuminated one of the important ways that cells respond to stress. The findings could also be relevant to Alzheimer’s, ALS and other diseases in which this mechanism may be abnormally active.
When stressed by heat, toxins or other potentially damaging factors, cells gather many of their messenger RNAs (mRNAs), molecules that carry the instructions for making proteins, into droplet-like compartments called stress granules. These granules sequester affected mRNAs, preventing them from being translated into proteins. The resulting slowdown in protein production helps the cell conserve energy, declutter and focus on repairs.
In the study, which appeared Sept. 14 in Nature Structural and Molecular Biology, the researchers confirmed that a tiny chemical modification on mRNAs, known as m6A, is key to the formation of stress granules.
“We were able to show that m6A has a primary role in driving mRNAs into these granules during cell stress,” said study senior author Dr. Samie Jaffrey, the Greenberg-Starr Professor of Pharmacology at Weill Cornell Medicine.
The study’s first author, Dr. Ryan Ries, was a Weill Cornell Graduate School of Medical Sciences doctoral student during the research.
Understanding How Stress Granules Form
Stress granules contain many different mRNAs from the cell, but not a random selection. Dr. Jaffrey and his team previously showed that mRNAs that are found in stress granules are often chemically tagged with a small cluster of atoms called a methyl group which attaches to adenosine, one of the mRNA building blocks. The resulting mRNA has regions that are enriched in N6–methyladenosine, or m6A. They also found that m6A-rich regions bind to YTHDF proteins—the more m6A an mRNA has, the more YTHDF proteins are present. The large amount of YTHDF proteins is needed to allow the m6A-mRNA–YTHDF complexes to accumulate into stress granules.
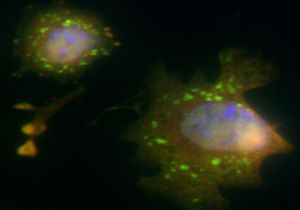
This image shows stress granules (green) that have formed throughout the cytoplasm of stressed cells.
Dr. Jaffrey and others assumed that m6A wasn’t the only factor directing mRNA into stress granules because longer mRNAs are also overrepresented. “We had thought that mRNA length was another factor, which is plausible since longer mRNAs have a tendency to stick to other mRNAs and form aggregates,” Dr. Jaffrey said.
However, in this study, when the researchers engineered cells that couldn’t form m6A and induced stress granule formation, they found that longer mRNAs weren’t overrepresented in the granules anymore. Dr. Jaffrey concluded that the m6A in the long mRNAs, and not mRNA length per se, was the key factor making longer mRNAs disproportionately abundant in stress granules.
Why Do Longer mRNAs Dominate Stress Granules?
During protein production, mRNAs are assembled in the nucleus of a cell from smaller regions of RNA called exons. The researchers observed that m6A is added to mRNAs as soon as the mRNAs are made in the nucleus. They also discovered that exons that were unusually long strongly triggered m6A formation in the corresponding mRNA. These long exons tend to be in long mRNAs, which explained why long mRNAs have high levels of m6A, and therefore are more likely to join stress granules, compared to mRNAs that are composed of only short exons.
Why does it benefit a cell to sequester longer mRNAs during episodes of cell stress? Dr. Jaffrey and colleagues speculate that in the distant evolutionary past, longer mRNAs were more likely to be dysfunctional or even from viruses. The development of cellular pathways to direct m6A-mRNAs into stress granules may have originated as a way to lock up these suspect mRNAs and prevent them from making unsafe proteins—though that process now appears to have evolved into a broader stress-response function.
While the new finding significantly advances the understanding of the basic biology underlying m6A and stress granule formation, it may also be relevant to neurodegenerative diseases.
“Maybe the abnormal stress granules that are formed in neurodegenerative diseases such as Alzheimer’s and ALS are driving those disease processes by chronically trapping beneficial m6A-containing mRNAs,” Dr. Jaffrey said. “We hope to find out whether blocking that mRNA-trapping process will help reverse pathology in these neurons.”
Many Weill Cornell Medicine physicians and scientists maintain relationships and collaborate with external organizations to foster scientific innovation and provide expert guidance. The institution makes these disclosures public to ensure transparency. For this information, see the profile for Dr. Samie Jaffrey.
Research reported in this newsroom story was supported by the National Institutes of Health grants R35NS111631, R01CA186702 and S10 OD030335.



